|
It could be conducted at a diagnostic clinic in the hospital eye service, at a diagnostic hub or mobile unit in the community or in primary care optometry enhanced services. If not available within the DES setting, the right ‘place’ for OCT capture will depend on local arrangements and availability of resources, such as the imaging equipment, connectivity and commissioning arrangements. 
Alternatively, it can take the form of an asynchronous virtual clinic after undertaking a non-medical (usually technician-led) OCT diagnostic assessment. 
Integration of OCT imaging into patient pathways can be directly made into the screening programme itself, ideally within the same appointment as the screening assessment, which is the most patient-centred pathway. In addition, patients with low-risk maculopathy below treatment levels should be monitored in OCT-supported assessments outside of routine medically led secondary care clinics. Referral to / assessment in secondary care face to face treatment clinics should NOT be accepted for any patient with diabetic maculopathy grading of M1 or above without an OCT scan and assessment of images to filter referrals. Where possible, OCT should be made available within the same appointment as the diabetic screening assessment for efficiency, patient convenience and to reduce patient anxiety. The proposed guidance uses best available evidence to propose patients with DES diabetic retinopathy grading M1 or above should have integration of OCT within the DES pathways or as part of a referral refinement protocol prior to assessment in secondary care treatment clinics, in addition to the current fundus photography. This guidance applies to those 18 years and over. Therefore, the use of OCT in diabetic maculopathy referral refinement pathways would reduce unnecessary referrals to HES. However, these changes have not been adopted in England at present. NHS Scotland introduced the inclusion of OCT surveillance in DES in January 2021. As retinal thickness is essential to make a clinical decision on treatment but cannot be accurately judged with 2D colour fundus image, an OCT is required to decide on treatment.Ĭurrent protocols in DES are significantly variable by geography with regards to OCT use. Individuals with non-central DMO or CRT <400μm may also be suitable for macular laser treatment. 
NICE recommends active treatment of DMO with licensed intravitreal injections in eyes with CRT of 400 μm or more. Thresholds for treatment are based on OCT measures of CRT. It allows accurate detection of DMOĪnd quantification of the degree of oedema through the measure of the central retinal thickness (CRT). OCT is a non-invasive imaging tool, using light waves to take high resolution cross-sectional 3D images of the retina. However, in DMO, leaked fluid builds up at the macula (the central part of the retina) causing swelling/elevation which is difficult to detect on a 2D image. Referrals to HES are made if there is a grade of R2 (preproliferative diabetic retinopathy) or R3 (proliferative retinopathy) and/or M1 (diabetic macular oedema/DMO) on the 2D colour fundus image. DES services are commonly held in the community or primary care with agreed criteria for referral to HES. Every diabetic person in the UK is required to attend (at minimum) an annual Diabetic Eye Screening (DES) where a 2D colour fundus (retina) image is taken. 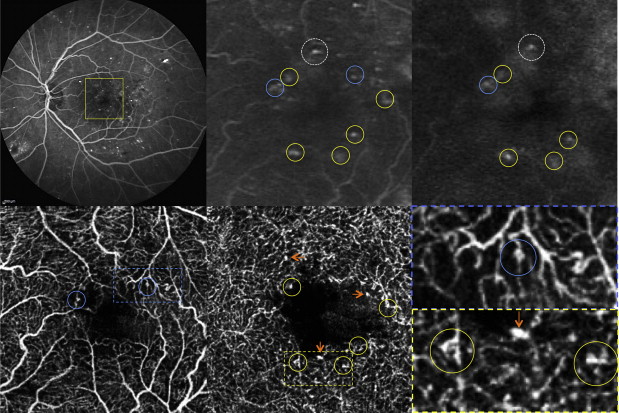
The best way of preventing visual loss in patients with diabetes is early detection and treatment. Diabetic macular oedema (DMO) is the leading cause of blindness in young adults in developed countries.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |

 RSS Feed
RSS Feed
